Food insecurity is an oft-overlooked underlying factor that can lead to preventable chronic diseases.
Too Little to Eat =Too Little to Be Healthy

Public health is a science concerned with protecting and improving the health of populations, whether in a neighborhood or an entire country. From a conventional viewpoint, public health focuses on promoting health and stopping disease—especially preventable ones such as heart disease, type 2 diabetes, and obesity. According to America’s largest public health agency, the Centers for Disease Control and Prevention (CDC), public health professionals work to limit health disparity by detecting, responding to, and preventing various diseases and promoting equity in healthcare. Consequently, much emphasis has been placed on educating consumers on lifestyle and dietary choices that are associated with preventable diseases. Although this approach is important and necessary, it assumes that people are in control of most of the factors that lead to unintended health consequences—particularly dietary choices. What if they aren’t? In fact, an overlooked factor associated with type 2 diabetes, obesity, and mental health problems is not a conscious choice for 12% of the U.S. population: food insecurity.
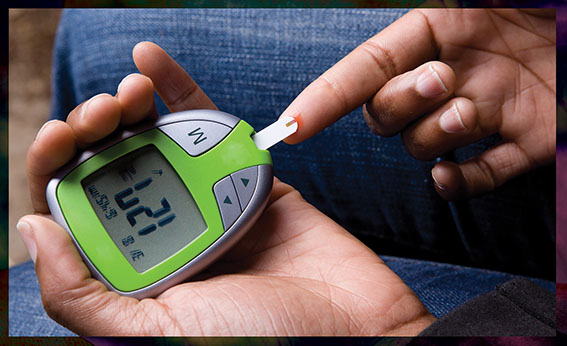
Food insecure individuals have up to a 50% higher risk of developing type 2 diabetes, and food-insecure diabetics may have to choose between purchasing medicine and supplies or buying groceries. © MarkHatfield/iStock/Getty Images Plus
Perennially, food insecurity is one of the country’s most poorly addressed public health issues, reliant on underfunded government policies and the generosity of U.S. citizens to address the problem. Food insecurity is defined as the disruption of food intake or eating patterns because of a lack of resources. The U.S. Department of Agriculture (USDA) has further distinguished two categories of food insecurity: low food security and very low food security. People who fall in the low food security category experience multiple instances of problems acquiring food and have a reduced diet quality. Individuals who have very low food security have multiple instances of reduced food intake and experience disrupted eating patterns because they could not afford to purchase food. Very low food security in the United States is usually intermittent rather than constant.
Programs That Address Food Insecurity
Through its Food and Nutrition Service, the USDA has 15 nutrition assistance programs in place to help low-income individuals feed themselves and their families. The largest of these programs is the Supplemental Nutrition Assistance Program (SNAP). SNAP provides resources to low-income families so that they can purchase food and move toward self-sufficiency. In fiscal year 2018, SNAP benefits averaged $1.40 per person per meal. SNAP benefits can be used to purchase vegetables; fruit; dairy products; meat, poultry, and seafood; breads and cereals; and snacks and nonalcoholic beverages. The program prohibits the purchase of alcoholic beverages, tobacco products, medicine, vitamins, and supplements but permits the purchase of soda, candy, cookies, potato chips, snack crackers, and other calorie-dense foods. The objective of SNAP is to ensure that no one in the United States goes hungry, but the program’s eligibility requirements are counterintuitive to its goal (Moran 2018, Wheaton 2019): In addition to imposing certain resource and income limits, the program has work requirements (with exemptions for people caring for one or more children under six years of age, elderly persons, people with a physical or mental disability, pregnant women, and a few other exceptions) and emphasizes “the importance of work and responsibility” (USDA 2019a). The work requirements are even stricter for low-income individuals categorized as able-bodied adults without dependents (ABAWDs) because of recent changes outlined in a new rule enacted by the Trump Administration. Beginning April 1, 2020, these changes will position SNAP as a program that offers assistance in difficult times but not as a way of life. In response to the fact that there are more than 36 million people receiving SNAP benefits while the unemployment rate is less than 4%, the new rule will also put greater limitations on each state’s ability to extend SNAP benefits beyond the certification period (this will restrict states’ ability to extend SNAP benefits beyond three months for every three-year period for ABAWDs). Of the new rule, U.S. Secretary of Agriculture Sonny Perdue has said, “We need to encourage people by giving them a helping hand but not allowing it to become an indefinitely giving hand. Now, in the midst of the strongest economy in a generation, we need everyone who can work, to work” (USDA 2019b). However, critics point out that work requirements do nothing to help unemployed low-income people find work (particularly ABAWDs who reside in areas with high employment rates, who have undiagnosed mental illness, who have criminal backgrounds, or who are homeless) and make it more difficult for these individuals to feed themselves and their families (Dean et al. 2018).
Food insecurity is more than a matter of public health; it is a matter of life and an early death.
Also among the nutrition assistance programs the USDA Food and Nutrition Service administers are the National School Lunch Program (NSLP), the School Breakfast program (SBP), and the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC). The NSLP and SBP are designed to provide nutritionally balanced no-cost or low-cost meals to eligible children each school day. And WIC provides nutritious foods to low-income pregnant and postpartum women and their children up to age five. WIC also provides access to resources such as health screenings (including immunizations) and nutrition counseling. In theory, the SBP, the NSLP, and WIC should reduce food insecurity by providing free breakfasts and lunches to school-age children living in food-insecure households and by assisting pregnant women and their young children with supplemental foods. In reality, the SBP and the NSLP are only beneficial to children living in food-insecure households during the months when school is in session. Moreover, the participation of food-insecure individuals in each of these programs has declined over time: The number of participants in WIC has declined by 26% since 2010, participation in the NSLP has declined by 7% since 2013, and the SBP experienced its smallest increase in participants since 1982 (Oliveira 2019). Undoubtedly, the improving economy is a contributing factor for the decline in nutrition assistance program enrollees, but analysts suspect that the Trump Administration’s restrictions (i.e., work and immigration-status requirements and stricter limitations for ABAWDs) on food assistance are also having an effect (Rosenbaum and Keith-Jennings 2019, Kelly 2019).
A Bleak Outlook

Studies have shown that fast-food chains and convenience stores outnumber full-service supermarkets in low-income neighborhoods. © stevegeer/iStock/Getty Images Plus
As a consequence of requirements, restrictions, and limitations of various federal nutrition assistance programs, individuals experiencing food insecurity tend to be caught in a bleak cycle that involves limited or no access to employment, transportation, full-service supermarkets, and so on. The phenomenon can begin with difficulty finding employment that pays more than the minimum wage or having no employment at all. This compels people to live in low-income housing located in neighborhoods where access is limited or nonexistent to services others take for granted. Moreover, when a household’s income is limited, families must choose between paying rent, utilities, medical expenses, and other bills or buying food. If paying bills is prioritized, then there may be little or no money left for food purchases. All of this triggers an undercurrent of stress, which some food-insecure individuals cope with by engaging in suboptimal dietary behaviors, such as purchasing and consuming inexpensive calorie-dense and nutrient-poor foods that are highly processed (e.g., fast food, chips and other snack foods, sweets, soda and other sugary beverages, etc.), and substance dependency (Weinfield et al. 2014, Davison et al. 2018, Whittle et al. 2018). In fact, according to the most recent Hunger in America study, 79% of food-insecure households purchase inexpensive unhealthy food to feed their families (Weinfield et al. 2014). Some food-insecure households’ reliance on poor food choices may be the result of living in communities with few or no full-service supermarkets, limited transportation options, and/or ubiquitous fast-food restaurants. Various studies have pointed out that fast-food chains and convenience stores outnumber full-service supermarkets in low-income neighborhoods, neighborhoods whose permanent residents are predominantly low-income blacks or low-income Latinos, and rural areas (Schneider 2015, Cooksey-Stowers et al. 2017, Florida 2018). In such vicinities, food-insecure individuals must travel further to purchase nutrient-dense foods such as whole vegetables, fruits, and grains; seafood; and lean meats. However, while it is true that low-income neighborhoods tend to have fewer full-service supermarkets, it is unclear whether this plays a role in determining the food choices low-income, food-insecure individuals make.
Low Funds, Low Nutrients

According to a Feeding America survey, 58% of the households it serves have one or more family members with high blood pressure. © DNY59/E+/Getty Images
Because of their elevated intake of calorie-dense, nutrient-poor foods, individuals who are food insecure tend to be at greater risk of numerous health problems. In fact, many who seem to have less steady access to food are overweight or obese and/or suffering from diseases that are typically associated with overconsumption of calories (e.g., type 2 diabetes, heart disease, and kidney failure) as well as mental health issues. According to Feeding America’s 2019 Health Implications of Food Insecurity survey, 33% of the households the food network serves have one or more family members with type 2 diabetes, and 58% of the households it serves have one or more family members with high blood pressure (Feeding America 2019). The CDC indicates that a complex association exists between income level and obesity and varies according to gender and race, so researchers are not certain whether the relationship is causal or coincidental: For example, recent research indicates that for women, the prevalence of obesity is highest among low-income women, but for men, the prevalence of obesity is lowest among low-income men (Ogden et al. 2017). Still, no one disputes that low-income people are more disposed to obesogenic risk factors (e.g., high intake of low-nutrient foods, sedentary lifestyles, stress, etc.), which increase their risk for obesity (Weinfield et al. 2014, FRAC 2015). In adults, obesity is considered a risk factor for dementia, and a recent study found a strong association between food insecurity and anxiety, depression, suicidal thoughts, and other mental health problems in young adults (Nagata et al. 2019, Floud et al. 2020).

Research indicates there is a strong association between food insecurity and anxiety, depression, suicidal thoughts, and other mental health problems. © Rawpixel/iStock/Getty Images Plus
Experts have identified choline and the omega-3 fatty acids docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) as key nutrients for healthy brain development. But children and young adults experiencing food insecurity may have deficiencies in these and other key nutrients, which could have far-reaching consequences for not only their physical development but also their minds and behavior. The human brain undergoes rapid development throughout childhood and continues developing until the mid-20s. Scientists and mental health professionals have known for some time that inadequate nutrition has a profound influence on neurocognitive development and mental health. The diet-mind connection encompasses not only the onset and severity of mental illness but also the expression of personality, mood, and behavior. For example, inhibitory control early in life predicts important life outcomes such as physical health, substance dependence, stability of personal finances, and participation in criminal activity (Moffitt 2011, Jentsch and Pennington 2014, Anzman-Frasca et al. 2015).
According to studies conducted by University of Illinois professors Anne Walk and Naiman Khan, lutein and zeaxanthin levels measured in the eye are correlated to measures of cognitive control and performance on academic achievement tests. Children with greater macular pigment optical density (MPOD)—the measure of the lutein/zeaxanthin status in the eyes and brain—tend to have greater intellectual ability and greater self-control (as well as better eye health) (Walk et al. 2017). In the Health, Aging, and Body Composition Study, researchers also determined that MPOD is positively associated with better cognition in older populations (Vishwanathan 2014). Most humans, regardless of income level, do not consume adequate levels of carotenoids, so their MPOD levels are low; in low-income children, MPOD levels are likely even lower. It appears that the brain may prefer lutein to other carotenoids; the body has a filter system that selectively retains and utilizes only some carotenoids in the body (Stringham et al. 2019). Lutein thus potentially has implications for cognitive health across the lifespan. Addressing food insecurity is thus not only vital to alleviating hunger but also a matter of improving the health and mental capacity of millions of Americans.

Many participants of U.S. nutrition assistance programs rely on food banks and food pantries to get by. © SDI Productions/E+/Getty Images
Foods that contain lutein and zeaxanthin include green leafy vegetables (kale, spinach, Swiss chard, dandelion greens, etc.), eggs, red pepper, broccoli, brussels sprouts, celery, summer squash, and asparagus. The best food sources of choline are beef, dairy products, seafood and chicken; seafood is the best source for DHA and EPA. Many of these foods are not high among the purchases made by participants in USDA nutrition assistance programs nor are they abundantly available through charitable food assistance programs (i.e., food banks and food pantries) (Garasky et al. 2016, Simmet et al. 2017). Even if such foods were more readily accessible in low-income neighborhoods, some individuals would avoid them because certain foods are unfamiliar and they don’t know how to prepare them (Fish et al. 2015).
A Path Forward
While food insecurity exists to some extent in every country around the world, it seems inconceivable that nearly 12% of the population of the United States (i.e., nearly 40 million people)—the eighth richest country in the world—experiences it. The U.S. government has a number of nutrition assistance programs in place, but the eligibility criteria and work requirements can be prohibitive for some low-income individuals. The combination of food insecurity and poor access to healthcare services translates to low-income individuals in the United States suffering from not only hunger and despair but also physical conditions that either impair their ability to thrive or shorten their lives. In essence, food insecurity is more than a matter of public health; it is a matter of life and an early death (Chetty et al. 2016, Alcott et al. 2019).
Fortunately, a large network of charitable food assistance programs throughout the United States provides food to those in need without requiring them to fill out forms or meet a list of requirements. Still, eradicating food insecurity and the medical and mental health problems associated with it may require more than just making it easier for low-income populations to obtain food (Szejda 2016, Alcott et al. 2019). It may also require educating low-income individuals about which foods make up a balanced diet, introducing them to nutritious foods with which they may not be familiar, and demonstrating how to prepare nutritious meals. Americans and U.S. policymakers may also benefit from observing and perhaps adopting other nations’ approaches to reducing food insecurity and improving the public-health outlook of low-income populations.
Toni Tarver is senior technical editor of Food Technology magazine (ttarver@ift.org).
REFERENCES
Alcott, H., J-P. Dube, and M. Schnell. 2019. “Eliminating Food Deserts Won’t Help Poorer Americans Eat Healthier.” The Conversation Dec. 1. http://theconversation.com/eliminating-food-deserts-wont-help-poorer-americans-eat-healthier-127295.
Anzman-Frasca, S., L. A. Francis, and L. L. Birch. 2015. “Inhibitory Control Is Associated With Psychosocial, Cognitive, and Weight Outcomes in a Longitudinal Sample of Girls.” Trans. Issues. Psychol. Sci.1(3): 203–216.
Chetty R., M. Stepner, S. Abraham, et al. 2016. “The Association Between Income and Life Expectancy in the United States, 2001–2011.” JAMA 315(16): 1750–1766
Cooksey-Stowers, K., M. B. Schwartz, and K. D. Brownell. 2017. “Food Swamps Predict Obesity Rates Better Than Food Deserts in the United States.” Int. J. Environ. Res. Public Health 14(11): doi: 10.3390/ijerph14111366.
Davison, K. M., C. Holloway, L. Gondara, et al. 2018. “Independent Associations and Effect Modification Between Lifetime Substance Use and Recent Mood Disorder Diagnosis With Household Food Insecurity.” PLoS ONE !3(1): doi: 10.1371/journal.pone.0191072.
Dean, S., E. Bolen, and B. Keight-Jennings. 2018. Making SNAP Work Requirements Harsher Will Not Improve Outcomes for Low-Income People. Center on Budget and Policy Priorities. Washington, D.C.
Feeding America. 2019. “Health Implications of Food Insecurity.” Online infographic. https://www.feedingamerica.org/sites/default/files/2019-05/2017-map-the-meal-gap-health-implications.pdf.
Fish, C. A., J. R. Brown, and S. A. Quandt. “African American and Latino Low Income Families’ Food Shopping Behaviors: Promoting Fruit and Vegetable Consumption and Use of Alternative Health Food Options.” J. Immigr. Minor. Health 17(2): 498–505.
Florida, R. 2018. “It’s Not the Food Deserts: It’s the Inequality.” CityLab, Jan. 18. https://www.citylab.com/equity/2018/01/its-not-the-food-deserts-its-the-inequality/550793/.
Floud, S., R. F. Simpson, A. Balkwill, et al. 2020. “Body Mass Index, Diet, Physical Inactivity, and the Incidence of Dementia in 1 Million UK Women.” Neurology 94(2): e123–e132.
FRAC. 2015. Understanding the Connections: Food Insecurity and Obesity. Food Research & Action Center, Washington, D.C.
Garasky, S., K. Mbwana, A. Romualdo, et al. 2016. Foods Typically Purchased by Supplemental Nutrition Assistance Program (SNAP) Households. U.S. Dept. of Agriculture, Food and Nutrition Service. Alexandria, Va. https://fns-prod.azureedge.net/sites/default/files/ops/SNAPFoodsTypicallyPurchased.pdf.
Jentsch, J. D., and Z. T. Pennington. 2014. “Reward, Interrupted: Inhibitory Control and Its Relevance to Addictions. Neuropharmacology 76: 479–486.
Kelly, M. 2019. “Have Trump’s Policies ‘Lifted’ Nearly 5 Million Americans Off Food Stamps?” The Washington Post, Feb. 20.
Moffitt, T. E., L. Arseneault, D. Belsky, et al. 2011. “A Gradient of Childhood Self-Control Predicts Health, Wealth, and Public Safety.” Proc. Natl. Acad. Sci. USA 108(7): 2693–2698.
Moran, R. L. 2018. “Why American Policy Is Leaving Millions Hungry.” The Washington Post, Aug. 7.
Nagata, J. M., K. Palar, H. C. Gooding, et al. 2019. “Food Insecurity Is Associated With Poorer Mental Health and Sleep Outcomes in Young Adults.” J. Adolescent Health 65(6): 805–811.
Ogden, C. L., T. H. Fakhouri, M. C. Carroll, et al. 2017. “Prevalence of Obesity Among Adults, by Household Income and Education — United States, 2011–2014.” MMWR 66(50): 1369–1373.
Oliveira, V. 2019. The Food Assistance Landscape: FY 2018 Annual Report. EIB-207. U.S. Dept. of Agriculture, Economic Research Service, Washington, D.C. https://www.ers.usda.gov/webdocs/publications/92896/eib-207.pdf?v=8949.8.
Rosenbaum, D. and B. Keith-Jennings. 2019. SNAP Caseload and Spending Declines Have Accelerated in Recent Years. Center on Budget and Policy Priorities. Washington, D.C.
Schneider, M. 2015. “Grocery Chains Leave Food Deserts Barren, AP Analysis Finds.” AP News. Dec. 7. https://apnews.com/8bfc99c7c99646008acf25e674e378cf.
Simmet, A., J. Depa, P. Tinnemann, et al. 2017. “The Dietary Quality of Food Pantry Users: A Systematic Review of Existing Literature.” J. Acad. Nutr. Diet. 117(4): 563–576.
Stringham, J. M., E. J. Johnson, and B. R. Hammond. 2019. “Lutein Across the Lifespan: From Childhood Cognitive Performance to the Aging Eye and Brain. Curr. Dev. Nutr. 3(7): doi: 10.1093/cdn/nzz066.
Szejda, K. 2016. “Will Requiring Food Stamp Retailers to Sell More Healthy Food Make It Easier for SNAP Recipients to Eat Better?” The Conversation, Mar. 23. https://
theconversation.com/will-requiring-food-stamp-retailers-to-sell-more-healthy-food-make-it-easier-for-snap-recipients-to-eat-better-55443.
USDA. 2019a. “SNAP Work Requirements.” https://www.fns.usda.gov/snap/work-requirements.
USDA. 2019b. “USDA Restores Original Intent of SNAP: A Second Chance, Not a Way of Life.” Press release, Dec. 4. U.S. Dept. of Agriculture, Washington, D.C.
Vishwanathan, R., A. Iannaccone, T. M. Scott, et al. 2014. “Macular Pigment Optical Density Is Related to Cognitive Function in Older People.” Age and Ageing 43(2): 271–275.
Walk, A. M., N. A. Khan, S. M. Barnett, et al. 2017. “From Neuro-Pigments to Neural Efficiency: the Relationship Between Retinal Carotenoids and Behavior and Neuroelectric Indices of Cognitive Control in Childhood.” Int. J. Psychophysiol. 118 (August 2017): 1–8.
Weinfield, N. S., G. Mills, C. Borger, et al. 2014. Hunger in America 2014: Executive Summary. Feeding America, Chicago, Il. https://www.feedingamerica.org/sites/default/files/research/hunger-in-america/hia-2014-executive-summary.pdf.
Wheaton, L. 2019. Estimated Effect of Recent Proposed Changes to SNAP Regulations. Urban Institute, Washington, D.C. urban.org.
Whittle, H. J., L. A. Sheira, E. A. Frongillo, et al. 2018. “Longitudinal Associations Between Food Insecurity and Substance Use in a Cohort of Women With or at Risk for HIV in the United States.” Addiction 114(1): 127–136.
Hero Image: © Nik_Merkulov/iStock/Getty Images Plus, © PeskyMonkey/iStock/Getty Images Plus
Authors
-
Toni Tarver
Categories
-
Food Health Nutrition
-
Food Policy
-
Dietary Guidelines
-
Obesity and Weight Management
-
Diet and Health
-
Food Technology Magazine



