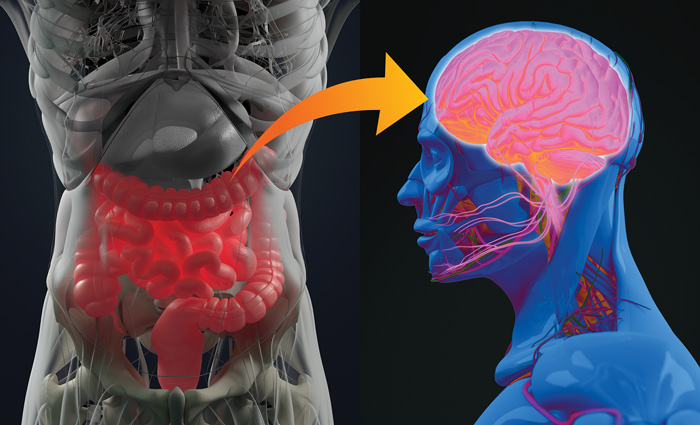
Feeding the Gut Microbiome
The microbes inhabiting our intestinal tract work in concert with our genes, the foods we eat, our environment, and other factors to influence our health and risk for disease.
Article Content
The poet Samuel Taylor Coleridge once described a metaphysical revelation as the discovery of “hidden worlds within worlds,” an analogy that could be applied to modern-day investigations into the human gut microbiome. Within the trillions of microorganisms that populate our gastrointestinal tract, more than 1,000 species of bacteria reside, along with millions of genes. Yet every person’s microbiome is unique, a fact that heightens the mystery surrounding the nature of the miniature ecosystem inside us.
Although studies of human gut flora have been taking place for centuries, it’s only recently that scientists have begun to delve into the complex relationship among gut health, diet, immune response, and disease. “Much of this [new research] is due to the molecular tools that were developed and continuously improved upon starting in the late ’80s, ’90s, and onwards,” explains Franny Gilman, director of research & development at TerraMax. “For quite some time, microbiology was constrained to studying what scientists could grow in the lab. With the advancements of these molecular tools (e.g., 16S rRNA gene work, the overall advancement in nucleic acid sequencing technologies, etc.), scientists can study microorganisms without growing them in a flask in the lab.”
In addition to molecular tools, another force driving new investigations into the microbiome are the interesting patterns that emerged from initial microbiome studies, many of which, says Gilman, have been instrumental “in revealing how prevalent, diverse, and how tightly interwoven microbial communities may be with host and ecosystem health.”
The correlation between overall health and gut health, in particular, has given rise to studies linking microbiome composition with a number of diseases, including obesity, neurological disorders, irritable bowel syndrome, autoimmune disease, and sleep disorders, to name a few.
“The microbiome has been associated with nearly every disease imaginable, but we’re still fairly short on mechanisms showing the microbiome is causal or even contributing to these conditions,” notes Tiffany Weir, associate professor in the Department of Food Science and Human Nutrition at Colorado State University. “I do think that we will eventually recognize just how important a healthy gut environment is to overall health, but at this point we have just scratched the surface.”
Another subject of ongoing study and debate is the effect of diet and lifestyle, with certain diets, including the Mediterranean, found to alter the gut microbiome in beneficial ways. Although such studies provide a foundation for future research, there is much that remains unknown about the complex interplay among gut composition, diet, and disease risk.
You Are What You Eat
“What we eat is what our microbes get to eat, so our diet largely shapes the membership of our gut microbiota,” says Purna Kashyap, scientific advisory board member of the American Gastrointestinal Association (AGA) Center for Gut Microbiome Research and Education.
Not only does our gut microbiota help to support our overall health, it is central to our ability to manage chronic diseases. According to pharmacist and author Sherry Torkos, the microbiome is integrally involved in digestion and nutrient absorption, and plays a role in the regulation of immune and neuroendocrine responses.
“The gut and immune system have a very close relationship,” she says, estimating that 70%–80% of immune cells are located in the gut. “Having a healthy microbiome is important for many aspects of immune health. Imbalances in the microbiota (dysbiosis) have been associated with inflammation and many chronic diseases. Diet plays a very significant role in the health of our microbiome—the food we eat provides nutrients to support both the growth and diversity of our microbiota. A diverse diet rich in prebiotic and probiotic foods is optimal.”
Indeed, a healthy diet is one of the best ways to promote a healthy microbiome—one that remains resistant to disease even through brief periods of poor dietary patterns. “In general, the gut microbiota is resilient and short dietary excursions will not cause permanent change; in fact, it will quickly go back to its original state,” explains Kashyap. “However, repeated insults like antibiotics, travel, [and] infections may eventually cause it to break.”
The Fiber Fix
One way to ensure a resilient gut microbiome is by eating a diet rich in fiber. “In general, high dietary fiber increases the diversity of the gut bacteria, and the more diverse a microbial community, the harder it is to disrupt it,” observes Kashyap. “So for now, we can only say increasing dietary fiber is good for maintaining a healthy microbiome. Just like other food groups, all dietary fiber is not created equal, and while we figure out what kind of fiber is good for what purpose, we can continue to recommend a high fiber diet in general.”
Of the many foods that are good sources of fiber, a number—including leeks, onions, and garlic—are also rich in prebiotics, the dietary compounds that feed the flora in our microbiome. In a rodent study undertaken at the University of Colorado at Boulder (Thompson et al. 2020), prebiotics were shown to influence gut metabolites that affect the brain, helping to reduce stress, promote sleep, and protect the microbiome from disruption. Although it’s unlikely that humans could consume enough foods high in prebiotics to get a better night’s rest, the study could be a first step in developing targeted therapeutics to ease stress.
At Washington University School of Medicine in St. Louis, scientists studying dietary fiber components are making headway in determining which types are best at promoting the growth of intestinal microbes associated with good health. The patterns emerging from the study (Patnode et al. 2019) provide an encouraging outlook for the possibility of one day producing microbiota-directed foods that selectively elevate the number of beneficial gut microbes. For now, food manufacturers are filling the void with an array of products that provide fiber in new and appealing ways.
Chicory root fiber is one example of an area ripe for new product development. Rich in inulin, chicory root acts as a prebiotic, helping to feed beneficial bacteria in the gut. Snack maker Lenny & Larry’s uses chicory root in its Complete Cookie line, which provides 16 grams of plant-based protein and a whopping 10 grams of fiber per cookie. Available in more than a dozen flavors, including Pumpkin Spice, Snickerdoodle, and Lemon Poppy Seed, the non-GM, vegan, soy- and dairy-free cookies are billed as being “better to your body while satisfying your sweet tooth.”
A Proliferation of Probiotics
In addition to fiber, diets rich in probiotics and fermented foods have been promoted as contributing to a healthy microbiome. Consumers looking to boost their digestive health are increasingly seeking out food and beverage products with specific functional claims, and manufacturers are responding.
Last year, Grand View Research projected the global probiotics market will reach $77.1 billion by 2025. As of 2018, probiotic beverages alone garnered revenues of $39.6 billion, reflecting a robust market despite the lack of conclusive evidence to support the benefits of probiotics.
“One of the most common myths is that we can fix a bad microbiome with probiotics, which has led to indiscriminate use of probiotics,” says Kashyap. “While there are some studies showing benefit of specific probiotics in a disease state, such as in antibiotic-associated diarrhea, for the vast majority there is no data showing clinical benefit. Probiotics are not a counter to overcome a bad diet, and the mainstay should be a healthy, balanced diet with sufficient dietary fiber.”
With the ongoing introduction of new probiotic-based products, consumers have more choices than ever when it comes to finding ways to enhance digestive health. “I think we will start to see a lot more probiotics supplemented into foods and beverages where they normally wouldn’t appear,” says Elaine Patterson, senior scientist, DuPont Nutrition & Biosciences. “There will be more consumer options for those that want to influence gut health. I also think we will start to see a lot more new diet types coming into practice, incorporating microbiome-influencing foods and supplements.”
Gilman believes that although new probiotic and prebiotic product formulations will continue to gain popularity among consumers, there’s reason to manage expectations. “Product developers should keep in mind that there’s no silver bullet, there won’t be one key product type, one key probiotic, one key prebiotic, etc., that will be linked to driving a healthy gut microbiome in all consumers. We harbor a diverse community of bacteria in our guts, and it makes sense that we likely need a diverse array of healthful inputs to keep those microorganisms happy. Further complicating the matter, there may be a lot of variation in healthy microbiomes. But in this variance comes more opportunity for a wider breadth of product development. This will create space for personalized consumer products.”
Torkos concurs. “Innovative companies recognize that probiotics are not a one-size-fits-all type of supplement,” she says, citing the newest generation of supplements from Wakunaga, which address various life stages from childhood to the senior years. “Products such as Kyo-Dophilus Kids, Daily and Fifty+, as well as formulas that combine other therapeutic ingredients such as Cran+ Probiotic (to support both bladder and digestive health) with various CFU (colony forming units) counts, give consumers the ability to choose the formula that works best for their health concerns.”
Boosting Immunity and Fighting Disease
One of the most promising areas of study for both research scientists and product developers is the role of the gut microbiome in immune response. Gilman believes that mounting evidence points to a link among the gut microbiome, immune system development, and overall immune responses. “The exact underlying mechanisms may still be unclear,” she says. “Some thoughts out there include that microbial by-products may bind to receptors in the gut lining leading to downstream effects, including immune responses.”
Kashyap observes that since gut bacteria help train the immune system during early life, they are vital players in the development of a healthy immune system. “We are now starting to test diet as a therapeutic in diseases like inflammatory bowel disease (IBD),” he says.
By studying diets with different combinations of fat, protein, and fiber, researchers hope to discern which combinations help keep inflammation in check. “One of the goals is to drive the gut bacteria to strengthen the intestinal barrier,” Kashyap explains, “which will prevent passage of harmful bacterial antigens across the epithelium—one way by which bacteria can trigger an immune response.”
At DuPont Nutrition & Biosciences, researchers are interested in the bidirectional communication pathway connecting the gut, the gut microbiome, and the central nervous system (CNS)—the microbiome-gut-brain axis. “The composition of the gut microbiota has been shown to be affected by stress and dietary manipulation—for example, through probiotic intervention—and has also been shown to modulate the stress response … ,” says Patterson.
She references a study in rats (Stenman et al. 2020) in which supplements of certain bacteria were administered to the rodents and shown to alleviate the negative effects of stress on gut microbiota composition and behavior. When 12 probiotic strains were compared, the effects were shown to be dependent on both species and strain. The promising results, says Patterson, “indicate that these strains could be effective in preventing chronic stress-related symptoms from developing, at least in the murine host. Whether these results can be translated to humans remains to be determined.”
“The largest hurdles that remain in nearly all microbiome studies include elucidating the underlying mechanisms,” observes Gilman. “Most current studies are correlating or linking certain patterns in the microbiome with health or disease. Can we go beyond that correlation and understand the mechanism of why that pattern is causing health or disease?”
A recent study by researchers at Weill Cornell Medicine (Chu et al. 2019) probed the question by drilling down to the molecular level to explore the mechanism behind gut and brain communication. Using mouse models, the scientists examined the effects of a depleted gut microbiota on brain chemistry. The results offer new insights into the interplay between chronic gastrointestinal conditions and mental health, as well as the role that chemicals derived from gut microbiota play in other diseases, such as depression, post-traumatic stress disorder, and Parkinson’s disease.
The Tailor-Made Diet
As new information comes to light about the link between diet and genetics, consumers are likely to become more interested in finding personalized solutions to reduce their risk for diet-related chronic disease. “Your gut microbiota is as unique to you as your fingerprint, and so I think personalized approaches will have to be considered down the line,” says Patterson.
A few companies are already using microbiome profiles to design customized approaches to nutrition. “The Weizmann Institute is doing some really solid work in this area,” says Weir, “and has developed a personalized diet company called Day Two. There are several other evidence-based personalized diets in the pipelines as well. I think it’s an exciting area but still has a ways to go for optimizing personalization for improved health.”
Day Two is designed to help individuals with diabetes manage their blood glucose. The approach was developed as a result of a five-year study conducted by the Weizmann Institute (Zeevi et al. 2015) and is built on a model that Weizmann says can more accurately predict glycemic response to foods and food combinations than counting carbohydrates. By coupling personal measures—such as an individual’s microbiome composition and data obtained from blood tests, questionnaires, anthropometrics, and food diaries—with artificial intelligence and machine learning, the program determines personal glycemic responses.
Gilman believes that personalized nutrition represents a unique area for product development as well. “I think this research will continue to fuel personalized medicine, and I think personalized consumer products will follow suit. Companies that perform personal microbiome tests already exist and may make diet recommendations …. I don’t see why a nutraceutical company or even a yogurt brand or granola bar brand couldn’t do something similar—slightly varied yogurt recipes, granola bar recipes, etc., that are tailored to the fingerprint of your microbiome. They could be designed to promote the current microbiome you have or maybe boost certain biomarkers. However, I think a lot of research would remain to show that the products drive the desired outputs.”
On the Horizon
Despite an increasing number of studies on the gut microbiome, its potential has yet to be fully tapped. “Just as our gut microbiome contains many different microbial species, we can expect that there are many ways these microbes influence intestinal and systemic function,” says Maria Marco, professor in the Department of Food Science and Technology at the University of California, Davis. “Now that we have a pretty good handle on which microbes are in the digestive tract, a next big goal will be to identify the specific cell products made by these microbes that can alter intestinal function and act distally at other sites on the human body.”
One of the areas that will see continued growth, believes Marco, is our knowledge about probiotics, prebiotics, fiber, and diet- and supplement-based approaches to altering the gut microbiome composition. “In order to take the science to the next level,” she says, “more large RCTs (randomized controlled trials) and observational studies will be needed as well as molecular studies designed to understand how gut microbiome-based approaches may work better for some people than others and which formulations work best.”
“We have a lot to learn, we need to better understand which specific bacterial strains exert a beneficial effect and, more importantly, how they do it, as until we understand the mechanism, it will be difficult to develop rational probiotics,” adds Kashyap. “We need better designed and controlled clinical studies done concurrently across multiple centers, and we need better standardization of methods. I think we have come a long way in a very short period; people forget that this is a very young field and it will take some time to answer some of the questions scientifically. We need to be careful not to try and skip the process just so we can meet the expectations from the field.”
Another area ripe for research, believes Weir, is food safety. “I think that there are a lot of things ‘hiding’ in the diet that can damage the gut microbiota and intestinal function,” she says. “We talk a lot about modifying the gut microbiota, but ultimately—if you are healthy—you want a stable microbiota that is resilient to perturbations. I think evaluating whether certain food additives disrupt microbial stability is important going forward. There is emerging research suggesting that emollients and other food stabilizers have detrimental effects on the gut barrier and microbiota. Evaluating ingredients for effects such as these will be important.”
Since research already shows that the gut microbiota is influenced by many factors, including diet, age, body weight, disease, mental disorders, exercise, medication, and sleep, Patterson believes that modifying it is also relatively simple, as its composition changes in response to various factors throughout life. “There is huge potential to exploit the malleability of the gut microbiota, and therefore it is seriously considered as a major modifiable factor contributing to our health,” she notes. “We are only at the tip of the iceberg towards discovering how we can harness the gut microbiota for our health, and the focus is broad. I’m biased, but right now I would say that the role of the gut microbiota in mental health, CNS function, and behavior is a hot topic, and major developments have been made towards understanding how the gut microbiota can influence mental disorders and mental health.”
REFERENCES
Chu, C., M. H. Murdock, D. Jing, et al. 2019. “The microbiota regulate neuronal function and fear extinction learning.” Nature 574: 543–548. doi.org/10.1038/s41586-019-1644-y.
McDonald, D., E. Hyde, J. W. Debelius, et al. 2018. “American Gut: an Open Platform for Citizen Science Microbiome Research” mSystems 3(3): e00031-18. doi: 10.1128/mSystems.00031-18.
Patnode, M., Z. Beller, N. Han, et al. 2019. “Interspecies Competition Impacts Targeted Manipulation of Human Gut Bacteria by Fiber-Derived Glycans” Cell 179(1): 59–73: E13. doi.org/10.1016/j.cell.2019.08.011.
Stenman, L., E. Patterson, J. Meunier, et al. 2020. “Strain specific stress-modulating effects of candidate probiotics: A systematic screening in a mouse model of chronic restraint stress” Behav. Brain Res. 379: 112376. doi: 10.1016/j.bbr.2019.112376.
Thompson, R.S., F. Vargas, P. Dorrestein, et al. 2020. “Dietary prebiotics alter novel microbial dependent fecal metabolites that improve sleep” Sci. Rep. 10: 3848. doi.org/10.1038/s41598-020-60679-y.
Zeevi, D., T. Korem, N. Zmora, et al. 2015. “Personalized Nutrition by Prediction of Glycemic Responses” Cell 163(5): 1079–1094. doi.org/10.1016/j.cell.2015.11.001.